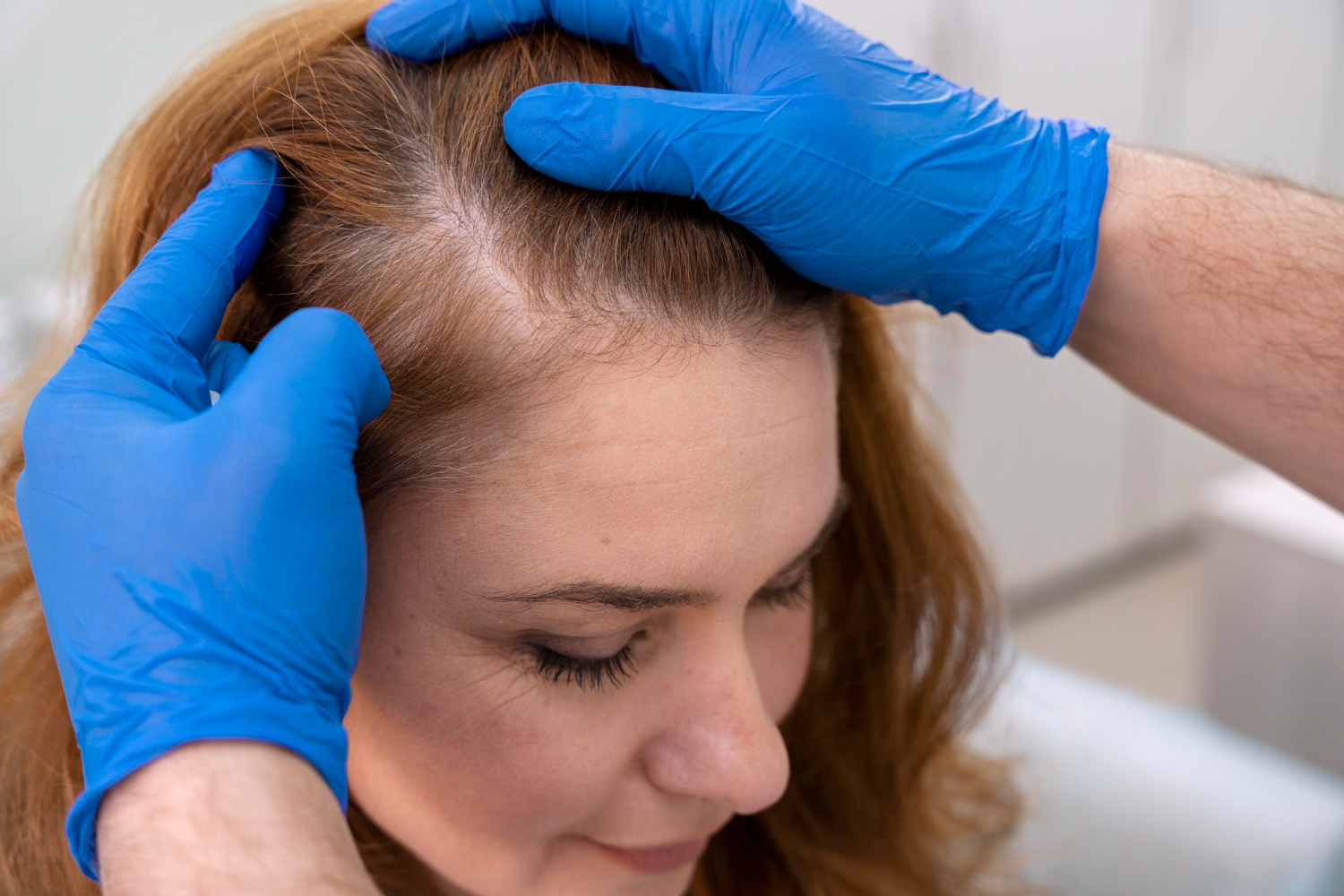
You pull your brush through your hair. More strands than usual come out. Or maybe you just notice your part looks wider. Your ponytail feels thinner.
If you're in your 40s or 50s, this is more common than you might think. And it can come from several directions at once.
This post breaks down the most common reasons women lose hair in midlife and what options may help.
Key Takeaways: What Could Be Causing Middle-Aged Hair Loss?
- Hair thinning after 50 is common. It can be linked to hormones, stress, nutrition, or other factors.
- If you're using a GLP-1 medication, rapid weight loss may play a role. This type of hair loss is usually temporary.
- Several options exist, from nutritional changes to topical or oral treatments, depending on the cause.
- A licensed healthcare provider can help you figure out what's driving it.
Ready to take the next step in your health journey? See how Get Thin MD works.
[BIG CTA GRAPHIC/BUTTON HERE]
Why Hair Thins After 50
Hair loss in midlife is rarely caused by just one thing. Most of the time, it's a mix of factors all happening at once.
Here are the most common reasons:
- Hormone shifts (especially estrogen and androgens)
- Nutritional gaps (low protein, iron, or zinc)
- Physical stress on the body (illness, surgery, or rapid weight loss)
- Emotional stress
- Thyroid issues
- Genetics
According to the American Academy of Dermatology, female hair loss affects up to 40% of women by age 50. That number goes up with age.
Is Hair Loss Caused By Hormones?
Hormones can play a role, especially during perimenopause and menopause. As estrogen levels drop, hair may grow more slowly and shed more easily.
At the same time, androgens (male hormones that everyone has) can become more active, which may contribute to follicle thinning over time.
The result is often hair that looks and feels thinner, especially at the crown and part line.
This type of hair loss is called female-pattern hair loss (androgenetic alopecia). It's the most common type in women.
What to Ask Your Licensed Healthcare Provider or Care Coach:
- "Is my hair loss connected to perimenopause or menopause?"
- "Should I check my hormone levels?"
- "Are there treatments that work with hormone changes?"
Could GLP-1 Be a Factor in Hair Loss?
If you're using a GLP-1 medication like compounded semaglutide or compounded tirzepatide, you may have noticed more hair shedding. This is more common than some people realize. But it's usually not the medication itself causing hair loss.
It's more likely a type of shedding called telogen effluvium.
Telogen effluvium means your body has been through physical stress. That stress pushes more hair follicles into a resting phase. Then they shed all at once, usually 2 to 4 months after the stress.
With GLP-1 medications, the "stress" is often rapid weight loss. Eating less can also mean less protein and fewer nutrients getting to your hair.
The good news: this type of hair shedding is usually temporary. Most people see it slow down or stop as their body adjusts.
What may help:
- Eating enough protein (aim for 1.2–1.6 grams per kilogram of body weight daily)
- Staying hydrated
- Taking a daily multivitamin or biotin supplement (check with your licensed healthcare provider first)
What to Ask Your Licensed Healthcare Provider or Care Coach:
- "Is my hair loss related to my weight loss speed?"
- "How much protein should I be eating?"
- "Do I need to check my nutrient levels?"
Have questions about GLP-1 medications and hair health? Get Thin MD's care team can help.
[BIG CTA GRAPHIC/BUTTON HERE]
When Stress Is the Culprit for Hair Loss
Stress—both physical and emotional—is one of the most overlooked causes of hair loss. When your body is under stress, it often shifts resources away from things like hair growth.
This can happen after:
- A major illness or surgery
- A period of very high emotional stress
- Significant weight loss
- Childbirth (though this is more common in younger women)
The tricky part: the shedding often shows up 2 to 4 months after the stressful event. So, it's easy to miss the connection.
Managing stress won't stop the shedding that's already happening. But it may reduce the chance of more cycles of loss.
Simple steps that may help reduce physical and emotional stress on your body:
- Getting 7–9 hours of sleep
- Eating regular meals with enough protein and healthy fats
- Gentle movement like walking or stretching
- Limiting alcohol and processed foods
What Actually Helps with Hormonal Hair Loss?
The right treatment depends on the cause. Here's a quick overview of what may help based on the underlying reason:
- Hormone-related loss: Talk to a licensed healthcare provider about hormone testing. Options may include hormone support or other treatments.
- Nutrition gaps: Increase protein. Check iron, zinc, and vitamin D levels. A registered dietitian can help build a plan.
- Telogen effluvium from GLP-1/weight loss: Give it time. Focus on nutrition. The shedding often slows on its own.
- Stress-related loss: Address the root cause when possible. Rest, nourish, and be patient with your body.
- Female-pattern hair loss: This type may need longer-term treatment. Topical or oral options exist.
Regardless of the cause, getting a blood panel is a smart first step. Low iron (ferritin), low vitamin D, and thyroid imbalances are common and easy to miss.
Oral Minoxidil: What to Know
You've probably heard of minoxidil—it's been used as a topical (applied to the scalp) treatment for hair loss for decades.
But there's growing interest in a lower-dose oral version (taken as a pill) for women.
According to research published by the Journal of the American Academy of Dermatology, low-dose oral minoxidil may help with several types of hair loss in women, including female-pattern hair loss.
A few things to know:
- It is a prescription medication, not available over the counter.
- It can take 3 to 6 months to see results.
- It must be used consistently to maintain results.
- It is not right for everyone—your licensed healthcare provider should review your health history first.
What to Ask Your Provider or Care Coach:
- "Is oral minoxidil an option for my type of hair loss?"
- "What are the risks and side effects?"
- "How long before I'd see results?"
Want support with your health goals—including nutrition and weight management? Start here.
[BIG CTA GRAPHIC/BUTTON HERE]
When to Talk to Your Licensed Healthcare Provider
Hair shedding that lasts more than 3 months is worth looking into. It's also time to check in if you notice:
- Patches of missing hair (not just overall thinning)
- Scalp irritation, redness, or flaking
- Hair loss that's getting worse, not better
- Other symptoms like fatigue, weight changes, or irregular periods
A licensed healthcare provider can check your thyroid, iron levels, hormone levels, and more.
For full safety details on GLP-1, hormonal therapies, and hair loss treatments, visit the Get Thin MD Important Safety Information page.
The Bottom Line
Hair thinning after 50 is common. And it's almost never caused by just one thing. Hormones, stress, nutrition, and weight changes can all play a role, sometimes at the same time.
The good news: many causes are treatable. And if you're on a GLP-1 medication, any extra shedding is often temporary.
Talk to your licensed healthcare provider to find out what's really driving it. The answer—and the right next step—may be simpler than you think.
Important Safety Information
Get Thin connects patients with licensed providers who may prescribe medication through state-licensed pharmacies. Prescription medication only available if prescribed after an online consultation, as applicable, with a healthcare provider. Physicians may prescribe compounded medications as needed to meet medical necessity or drug shortages. The FDA does not review or approve any compounded medications for safety or effectiveness. Results may vary. Please visit https://www.getthinusa.com/important-safety-information for important safety information.